If you’ve been dealing with unexplained bloating, fatigue, brain fog, or skin flare-ups, a food sensitivity test may finally connect the dots. Unlike a standard allergy panel, a food sensitivity test measures delayed IgG immune responses to common foods, revealing hidden inflammatory triggers that can take hours or even days to produce symptoms. Research published in the Journal of the American College of Nutrition estimates that up to 20% of the population may have undiagnosed food sensitivities, precisely because the delayed onset makes self-diagnosis nearly impossible.
In this guide, we break down exactly what a food sensitivity test measures, how it differs from allergy and intolerance testing, the symptoms to watch for, available testing options, and how to turn your results into a personalized action plan.
Ready to uncover your hidden food triggers? 1st Optimal’s comprehensive food sensitivity panels deliver clear, actionable data paired with expert-guided protocols. Book your free discovery call or call (816) 744-6814.
Understanding your methylation test results can also provide valuable insights into how your body processes nutrients and clears toxins.
What Is a Food Sensitivity Test and How Does It Work?
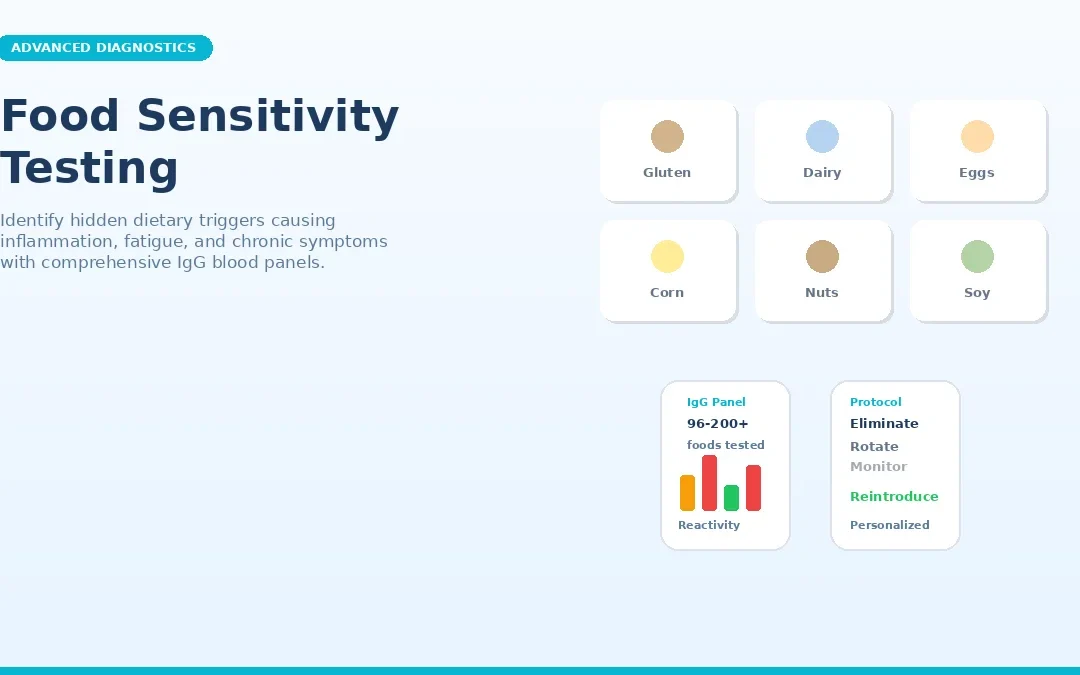
A food sensitivity test is a blood-based diagnostic that analyzes your immune system’s IgG antibody response to dozens, sometimes hundreds, of common foods. A small blood sample, collected via finger prick or standard draw, is sent to a lab where each food’s reactivity level is measured and reported as low, moderate, or high.
The goal is straightforward: identify which specific foods are provoking your immune system and contributing to chronic, low-grade inflammation. The results create a clear roadmap for an elimination protocol, which is the most direct path to symptom relief.
What makes a food sensitivity test distinct from other food-reaction tests is the type of immune response it measures. Food sensitivities involve IgG antibodies, which produce delayed reactions, anywhere from several hours to 72 hours after eating. This delay is the primary reason most people never connect their symptoms to a particular food without testing.
How Does a Food Sensitivity Differ from a Food Allergy or Intolerance?
These three terms describe fundamentally different biological mechanisms. Using them interchangeably leads to confusion and, often, the wrong testing approach.
Food allergies are IgE-mediated immune reactions. They produce immediate symptoms, typically within minutes to two hours, ranging from hives and swelling to life-threatening anaphylaxis. According to the American College of Allergy, Asthma, and Immunology, food allergies affect roughly 4% of adults and are usually lifelong. Standard diagnostic testing includes skin-prick tests and specific IgE blood panels.
Food intolerances are not immune-mediated at all. They result from enzyme deficiencies, the most common being lactose intolerance, where insufficient lactase prevents proper digestion of dairy sugars. Symptoms are primarily gastrointestinal (bloating, gas, diarrhea), dose-dependent, and limited to the digestive tract.
Food sensitivities sit between the two. They involve an IgG-mediated immune response that is delayed, systemic, and dose-dependent. Rather than a single dramatic reaction, sensitivities drive chronic, whole-body inflammation affecting digestion, cognition, skin, joints, and mood. Because symptoms are diffuse and delayed, food sensitivities are by far the hardest to identify without lab testing.

What Are the Most Common Food Sensitivities?
While any food can theoretically trigger an IgG response, certain foods appear on sensitivity panels far more frequently:
- Gluten — Found in wheat, barley, and rye. Non-celiac gluten sensitivity is now recognized as a distinct clinical condition, documented in BMC Medicine, that triggers systemic inflammation and neurological symptoms independent of celiac disease.
- Dairy — Both casein and whey proteins can provoke IgG responses. Dairy sensitivities often manifest as sinus congestion, acne, and digestive discomfort rather than the GI-only symptoms of lactose intolerance.
- Eggs — Whites and yolks can be tested separately; many people react to one but not the other.
- Soy — Ubiquitous in processed foods under names like soy lecithin, soy protein isolate, and vegetable oil.
- Corn — Corn-derived ingredients (maltodextrin, dextrose, high-fructose corn syrup) are present in thousands of packaged foods.
- Nuts and seeds — Almonds, cashews, and sesame are frequent triggers.
- Nightshades — Tomatoes, peppers, eggplant, and potatoes contain alkaloid compounds some individuals find inflammatory.
- Shellfish and certain fish — These can trigger both IgE allergies and IgG sensitivities.
Importantly, a positive sensitivity result doesn’t mean permanent elimination. With proper gut-healing protocols, many people successfully reintroduce reactive foods within 3-6 months.
What Are the Signs You Need a Food Sensitivity Test?
Because food sensitivity symptoms are delayed, low-grade, and systemic, they mimic dozens of other conditions. Here are the hallmark signs that food-driven inflammation may be at play:
Chronic digestive issues: Persistent bloating, gas, constipation, or diarrhea despite eating a “healthy” diet. When your gut never settles regardless of what you eat, hidden food sensitivities are a likely contributor.
Unexplained fatigue: Tiredness that sleep doesn’t resolve, especially post-meal energy crashes. A 2018 study in Nutrients linked elevated IgG food antibodies to significantly higher fatigue scores. The inflammatory cascade literally diverts metabolic energy toward immune activity, which is a phenomenon many women experiencing hormonal changes find compounds their existing exhaustion.
Brain fog: Difficulty concentrating, memory lapses, or word-finding problems. Neuroinflammation from dietary triggers directly impairs cognitive function, a pattern well-documented in the gut-brain axis literature.
Skin conditions: Eczema, acne, rosacea, or unexplained rashes. Research in Dermatology has connected IgG food reactions to chronic skin conditions. The skin is a downstream target of systemic inflammation.
Joint pain and stiffness: Inflammatory mediators from food sensitivities can accumulate in joint tissue, producing pain and stiffness that mimics early arthritis.
Mood disturbances: Anxiety, irritability, and depressive symptoms have been linked to food-driven inflammation via the gut-brain axis, an area of active hormonal health research.
Headaches and migraines: A study in Cephalalgia found that IgG-guided elimination diets significantly reduced migraine frequency in participants.
If several of these symptoms overlap and conventional workups have come back normal, a food sensitivity test is a logical next step.
Tired of guessing what’s causing your symptoms? 1st Optimal pairs food sensitivity testing with cortisol, DUTCH hormone, and comprehensive blood panels to find root causes, not band-aids. Schedule your consultation today.
What Types of Food Sensitivity Tests Are Available?
Several testing methodologies exist, each with distinct strengths:
IgG Blood Panel Testing
The most widely used approach. A blood sample is analyzed for IgG antibody levels against 96-200+ foods. Results are categorized by reactivity level, providing a clear starting point for elimination. Pros: Comprehensive, objective, tests many foods simultaneously. Cons: Measures immune exposure, which should be correlated with symptom tracking for full clinical relevance.
Elimination Diets
The gold standard for confirmation. Suspected trigger foods are removed for 2-6 weeks, then reintroduced one at a time while monitoring symptoms. Pros: Directly measures real-world response. Cons: Time-consuming, difficult to execute with multiple sensitivities, requires significant discipline.
MRT (Mediator Release Test)
Measures the release of inflammatory mediators (cytokines, prostaglandins) from white blood cells upon food exposure. Rather than measuring antibodies, it measures the downstream inflammatory result. Pros: Captures non-IgG pathways, includes food chemicals. Cons: More expensive, fewer practitioners offer it.
At-Home vs. Clinical Testing
At-home finger-prick kits have proliferated, but they typically lack the clinical interpretation that makes results actionable. A test result without expert guidance is just data. Working with a qualified functional medicine provider to interpret results and build a personalized protocol is what transforms numbers into outcomes.
How Do You Interpret Food Sensitivity Test Results?
Receiving a report showing dozens of reactive foods can feel overwhelming. Here is how to approach it strategically:
High-reactivity foods: Eliminate completely for 4-8 weeks. These are the most likely symptom drivers. This elimination window allows inflammation to clear and the intestinal lining to begin repairing.
Moderate-reactivity foods: Place on a rotation schedule, consuming no more than once every 3-4 days. This prevents further sensitization while you heal.
Low-reactivity foods: Generally safe to continue eating. Monitor for symptoms and reassess after the initial elimination phase.
Four principles for acting on results:
- Prioritize, don’t panic. Focus on the top 5-10 highest-reactive foods first. Removing everything simultaneously creates nutritional gaps.
- Keep a symptom journal. Track energy, digestion, mood, sleep, and skin daily during elimination. Patterns emerge quickly.
- Reintroduce methodically. After the elimination window, add one food back every 72 hours. This spacing catches delayed reactions.
- Address root causes. Sensitivities are often a symptom of gut dysfunction. Eliminating trigger foods without healing the gut risks developing new sensitivities, which is why pairing food sensitivity testing with metabolic and gut health assessments is critical.
How Does Gut Health Cause Food Sensitivities?
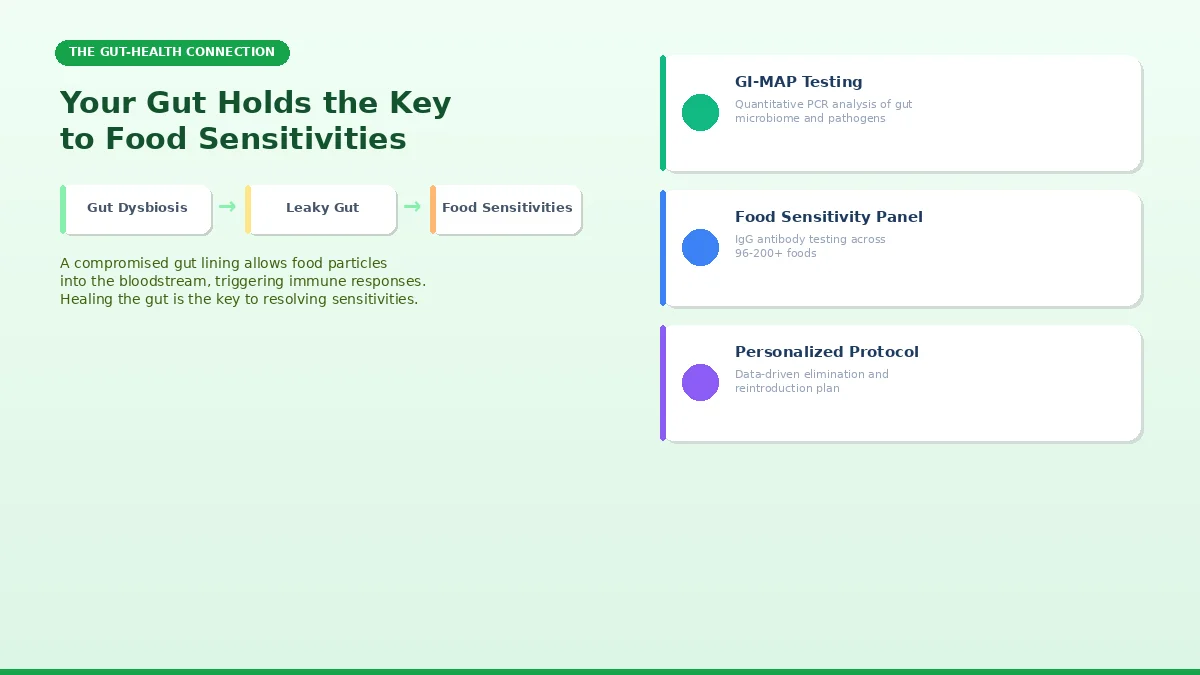
Food sensitivities rarely exist in isolation. In most cases, they signal underlying gut dysfunction, specifically intestinal permeability (“leaky gut”) and microbiome imbalances (dysbiosis).
The mechanism is well-established: when the tight junctions of the intestinal lining become compromised, partially digested food particles cross into the bloodstream. The immune system flags these particles as foreign and mounts an IgG antibody response. Over time, this creates a self-perpetuating cycle of inflammation and increasing reactivity. Research in Frontiers in Immunology has demonstrated that increased intestinal permeability is associated with a wide range of inflammatory and autoimmune conditions.
This is precisely why comprehensive gut health testing is essential alongside food sensitivity panels. The GI-MAP (Gastrointestinal Microbial Assay Plus) test uses quantitative PCR technology to map your gut ecosystem, identifying:
- Pathogenic bacteria, viruses, and parasites
- Beneficial bacteria populations (Lactobacillus, Bifidobacterium)
- Opportunistic organism overgrowth
- Digestive enzyme function and fat absorption markers
- Inflammatory markers including calprotectin and secretory IgA
- Intestinal permeability indicators
By layering GI-MAP data on top of food sensitivity results, your provider can build a protocol that addresses root causes: targeted probiotics, digestive enzyme support, gut-lining repair nutrients, and a phased reintroduction timeline. This approach doesn’t just remove trigger foods; it restores tolerance. The same principle applies to cortisol-driven gut disruption, where chronic stress compounds intestinal permeability.
How Does 1st Optimal Approach Food Sensitivity Testing?
At 1st Optimal, food sensitivity testing is one component of a comprehensive, data-driven diagnostic model. We don’t treat sensitivities in isolation, because they rarely exist that way.
Comprehensive testing panels: Our food sensitivity panels measure IgG reactivity across a wide range of common foods. We pair these results with DUTCH hormone metabolite analysis, cortisol and stress testing, and full blood panels to reveal the interconnected factors driving your symptoms.
Expert-guided interpretation: Your dedicated Membership Manager works with our medical team to translate raw data into a clear, prioritized action plan tailored to your symptoms, history, and goals.
Personalized elimination and reintroduction protocols: We design phased plans that eliminate confirmed triggers while maintaining nutritional completeness. This is a strategic protocol, not a generic “avoid these 30 foods” list.
Root-cause resolution: Because food sensitivities commonly stem from gut dysfunction, hormonal imbalances, or chronic stress, we investigate and address the underlying drivers. The goal is not lifelong avoidance; it is restoring your body’s balance and rebuilding food tolerance.
Telehealth convenience: Every step, from at-home test kits to provider consultations to protocol adjustments, happens through our fully virtual care model. No waiting rooms. No scheduling friction.
Get answers, not guesswork. 1st Optimal’s advanced diagnostic panels combine food sensitivity testing with hormone, cortisol, and gut health analysis for a complete picture. Book your free discovery call today or call (816) 744-6814.
Frequently Asked Questions About Food Sensitivity Tests
How accurate are food sensitivity tests?
IgG food sensitivity tests reliably measure immune reactivity to specific foods. Elevated IgG indicates an active immune response, but results should be correlated with symptoms for clinical significance. Professional interpretation and a guided elimination protocol are essential for translating test data into real health improvements.
How long until I feel better after eliminating trigger foods?
Most people notice initial improvements within 2-3 weeks. Significant symptom resolution typically occurs by 4-8 weeks. Full gut healing and tolerance restoration may take 3-6 months depending on the severity of underlying dysfunction.
Can food sensitivities go away?
Yes. Unlike true IgE food allergies, which are typically lifelong, food sensitivities are often reversible. By healing the gut lining, rebalancing the microbiome, and following proper reintroduction protocols, many people successfully resume eating previously reactive foods without symptoms.
What is the difference between food sensitivity testing and celiac testing?
Celiac disease is an autoimmune condition triggered by gluten that damages the small intestine. Celiac testing measures specific antibodies (tTG-IgA, DGP-IgA) and may require a biopsy. Food sensitivity testing measures broader IgG reactivity across many foods. You can be gluten-sensitive without having celiac disease.
Should I keep eating normally before my test?
Yes. Continue your normal diet before testing. IgG antibodies require recent food exposure to be detectable. If you’ve eliminated a food for several weeks, it may not appear on the panel even if you are sensitive to it.
How much does food sensitivity testing cost?
Costs vary by panel size and methodology. At 1st Optimal, food sensitivity testing is part of our comprehensive diagnostic approach. Your Membership Manager can provide specific pricing and help determine which panel aligns with your health goals. Contact us for details.
About the Author: Joe Miller is the CEO of 1st Optimal and a certified health professional with a Bachelor of Education in Kinesiology, Exercise Science, Health, and Nutrition. He holds a 2-Year Fellowship from A4M (American Academy of Anti-Aging Medicine), training from Worldlink Medical, ongoing BHRT certifications from A4M, NASM certification, NSCA CSCS credential, and American Council on Exercise accreditation. Connect on LinkedIn.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. The information provided is not intended to diagnose, treat, cure, or prevent any disease. Always consult with a qualified healthcare provider before making dietary changes, starting an elimination protocol, or beginning any new health program. Food sensitivity testing should be interpreted by a licensed medical professional in the context of your individual health history.